Steps for GP - hepatitis C shared care with Dr Samuel
- GPs, with no experience in HCV treatment, are eligible to prescribe Hepatitis C treatment under the PBS, provided it is done "in consultation with" a gastroenterologist, hepatologist or infectious disease physician experienced in the treatment of chronic Hepatitis C infection.
- For the purposes of prescribing the hepatitis C medicines through the PBS, the term "in consultation with" is intended to mean a GP must consult with one of the specified specialists by phone, mail, email or videoconference in order to meet the prescriber eligibility requirements.
- Patients do not need to have attended a specialist appointment prior to being prescribed one of the new medicines by a medical practitioner.
- Outside NSW and Victoria, GPs are the main providers of DAA treatments in Australia
- see: Hepatitis C fact sheet for community-based prescribers and General Statement for Drugs for the Treatment of Hepatitis C
Two options for shared care of your patient with Dr Samuel, either:
1. Remote written Hepatitis C treatment assessments with "remote pbs treatment approval":
- Assessments from GP's "remote pbs consultation form" not rooms consultation
- No cost to patients
- For local and remote GPs who are comfortable starting and or monitoring their patients during treatment according to the Australian Recommendations for the Management of Hepatitis C: A Consensus Statement updated 9/2018 (for summary see below)
- Please notify Dr Samuel of the HCV RNA result performed at least 12 weeks after completing treatment (gastromail+HCV@gmail.com)
2. Private rooms or videoconsultation including:
- standard specialist consultation with usual care
- on treatment specialist monitoring with Dr Samuel
- an experienced hepatitis C clinical nurse consultant (CNC) coordinating care
- educational mailouts to patients, on treatment monitoring until cure (usually out to week 12 post treatment)
- this may follow "remote pbs treatment approval" for on treatment monitoring
Hepatitis C treatment tips
1. Complete pretreatment assessment

2. Submit "remote pbs consultation form" to Dr Samuel's rooms
3. Starting treatment
Dr Samuel will review "remote consultation HCV shared care form" and reply (via email or fax) to referring doctor within 5 days, then streamlined authority script may be written and treatment started:
- if there is enough information provided, that Dr Samuel can agree with the treatment decision, he will send approval to referring doctor
- if further brief information is needed, Dr Samuel may request updated information for "form" and then approve treatment decision
- if "form" suggests a degree of complexity, Dr Samuel may suggest a consultation (video or rooms)
4. If video (with or without GP) or rooms consultation
if requested in addition to or in place of remote written pbs consultation , please confirm appointment with rooms:
- many GPs who are comfortable to manage hepatitis C patients on treatment and beyond may choose to have written pbs consultation only
- for a more active shared care arrangement (either before or after starting treatment) including a formal consultation and hepatitis C nurse consultant support for your patient, please refer the patient to the rooms or if you wish to be present via video please have your rooms coordinate a shared time.
Australian recommendations for the management of hepatitis C virus infection: a consensus statement to be updated 9/2018
tables produced by the expert panel representing the Gastroenterological Society of Australia (Australian Liver Association), the Australasian Society for Infectious Diseases, the Australasian Society for HIV, Viral Hepatitis and Sexual Health Medicine, the Australasian Hepatology Association, Hepatitis Australia and the Royal Australian College of General Practitioners
Goal of Treatment:
to reduce all-cause mortality and improve liver-related health outcomes with SVR12 (sustained virological response = virological cure)
SVR12 = HCV RNA undetectable > week 12 after completion of therapy. It is a durable endpoint in 99% of patients beyond 5 years. HCV antibodies remain detectable.
Who to treat?
all chronic HCV patients (except those with life expectancy <12 months that can not be remediated by treating HCV, by transplantation or other therapy
Benefits of cure
control hepatic necroinflammation
- improved ALT/AST levels
- slow rate of liver fibrosis progression
- improvement in liver fibrosis and necrosis (>40% at 20 months)
- resolution of cirrhosis (50% at 20 months)
reduce symptoms and mortality from extrahepatic manifestations including:
- cryoglobulinemic vasculitis
- renal disease
- NHL
decrease cirrhosis complication
- improvement in portal hypertension, splenomegaly etc
- 70% decrease risk of hepatocellular carcinoma
- 90% decrease risk of liver-related mortality and liver transplant
improve qualities of life including physical, emotional and social health
- prevent progression to diabetes and complications
reduce fatigue
improve public health with reduced transmission
Work-up
A person could have hepatitis C if they are

Pre-treatment HCV workup
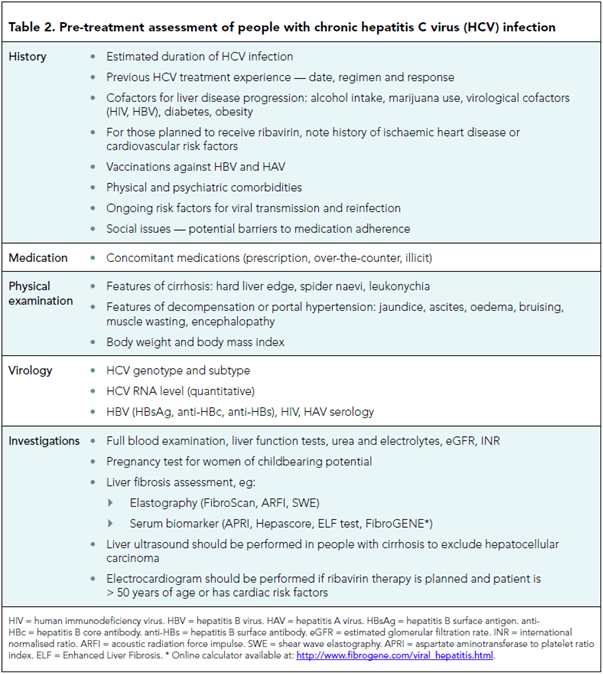
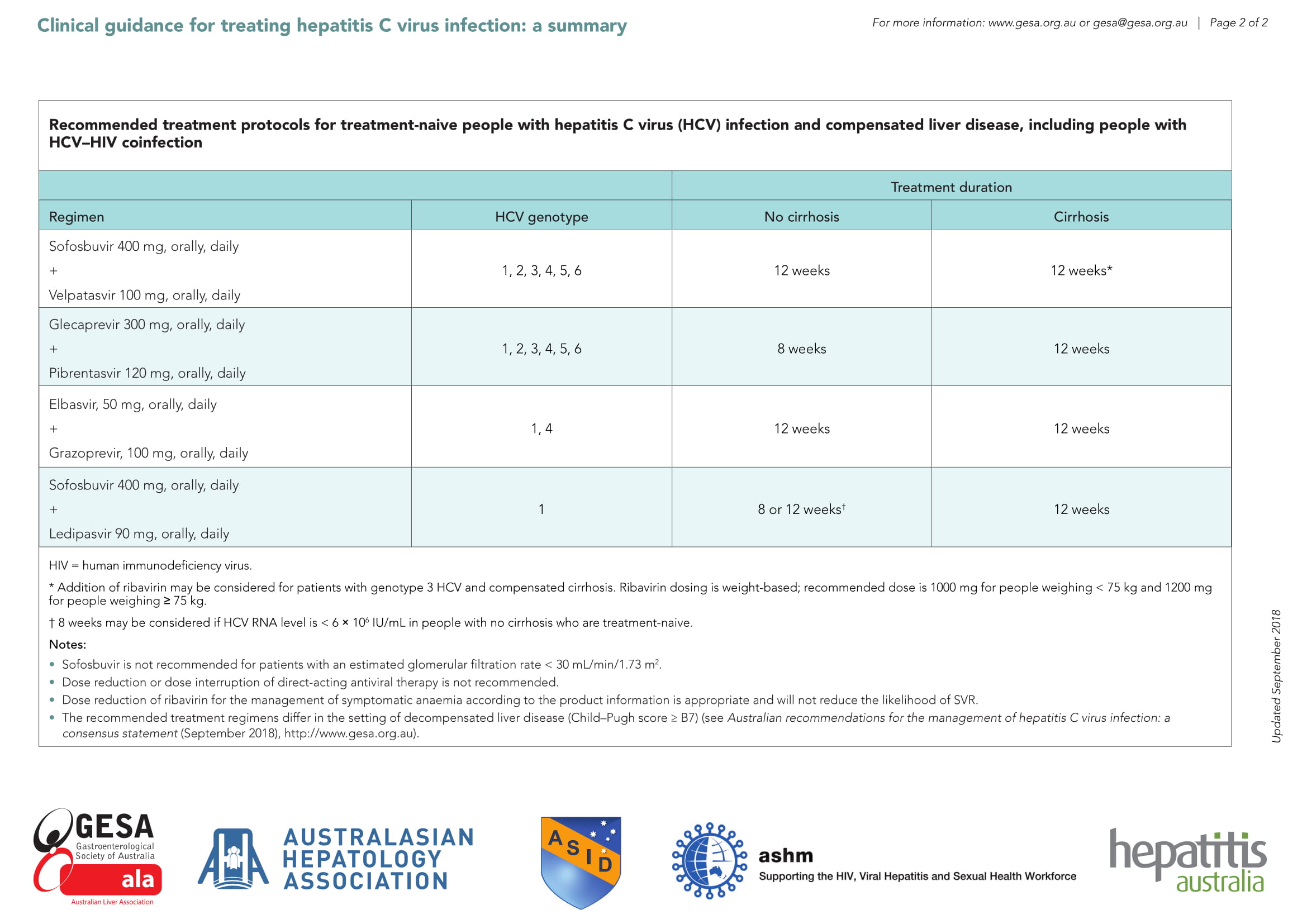
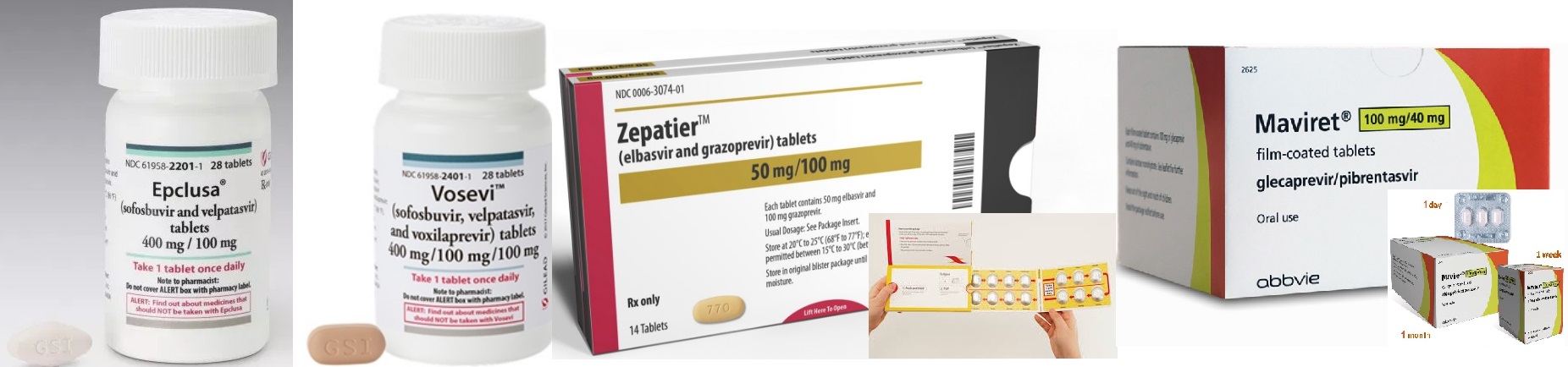
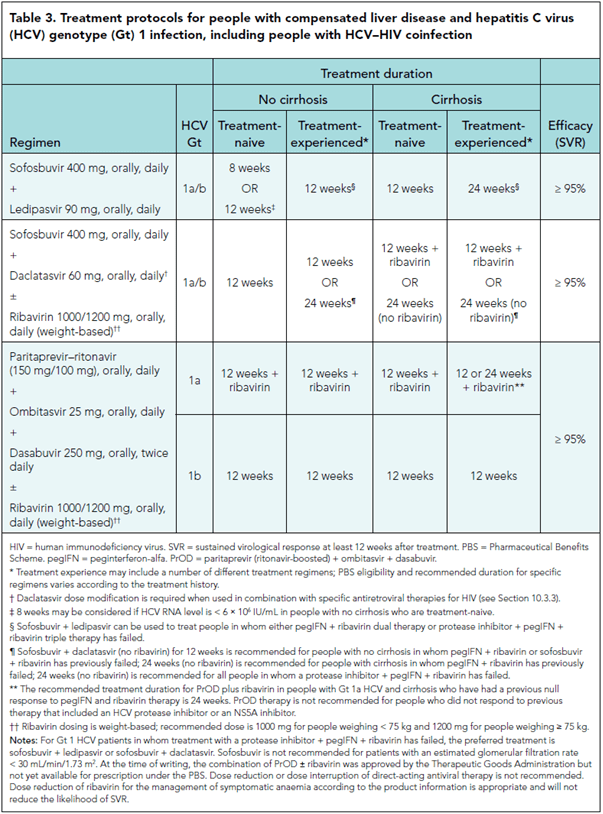
Treatment
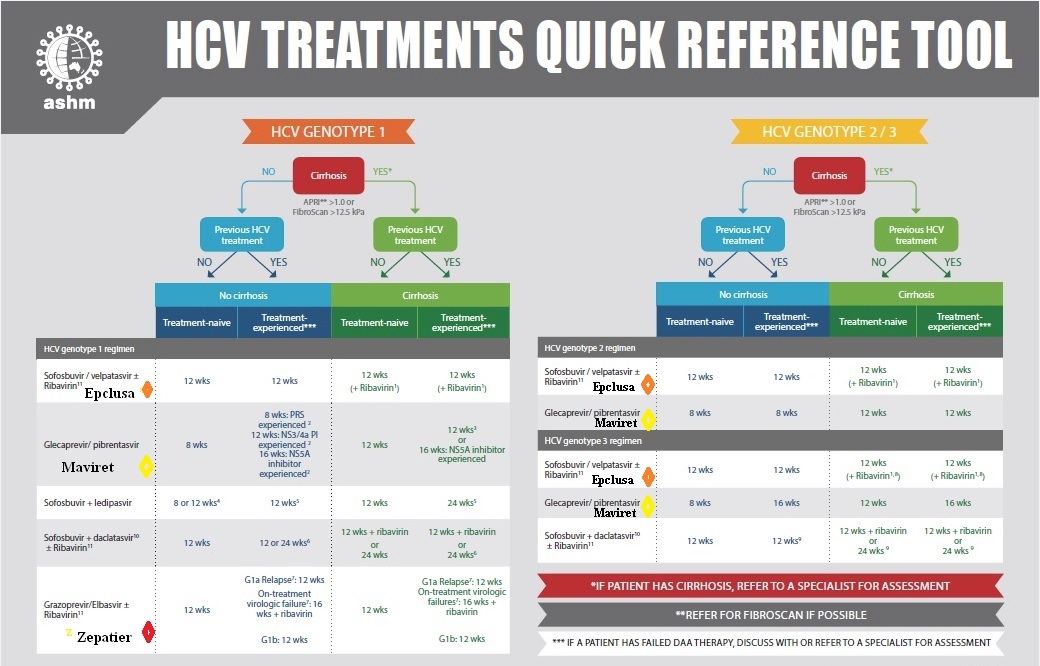
Genotype 1
Genotype 2-3
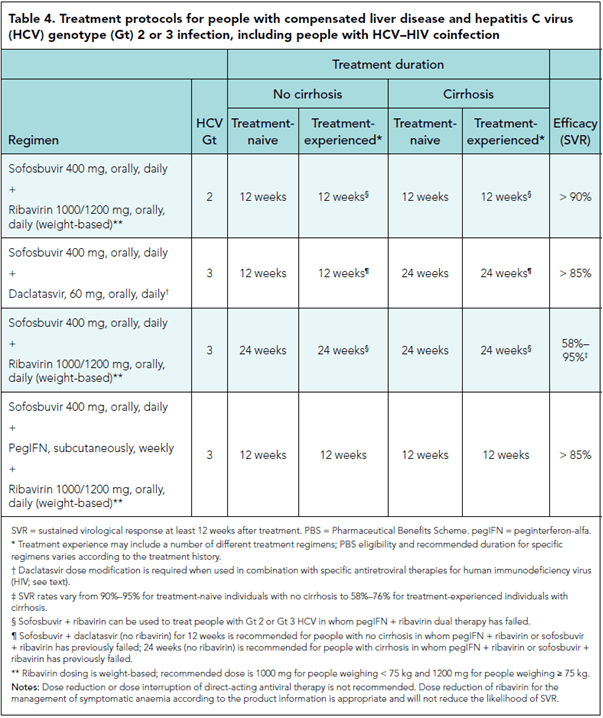
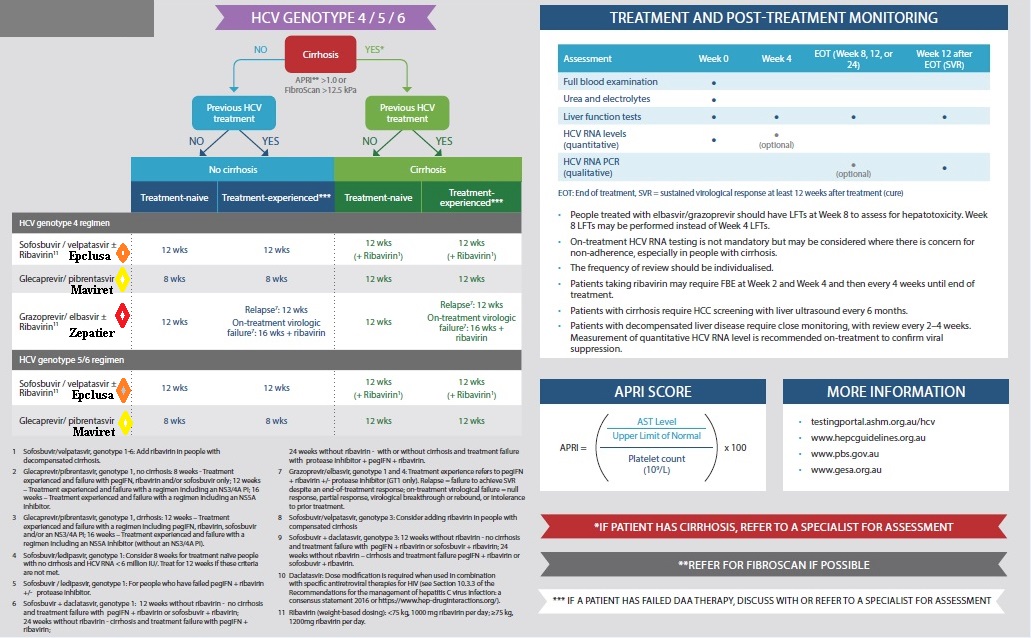
Genotype 4-6
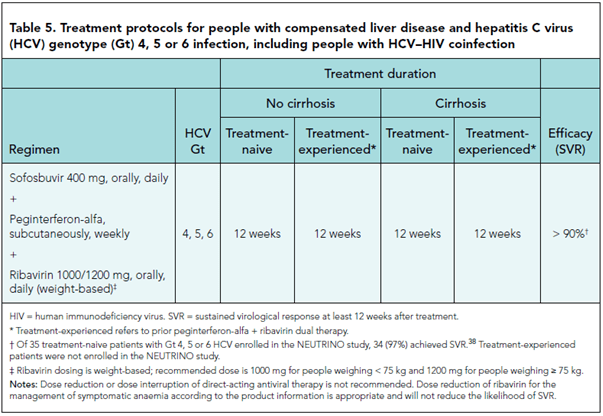
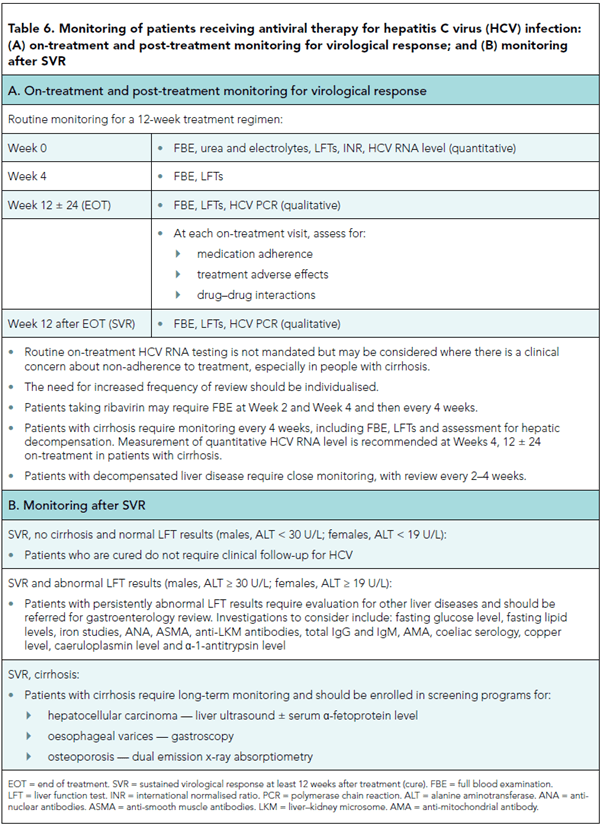
Monitoring
Monitoring - On treatment and post SVR