Detailed practical guidance
Understanding bile acid diarrhoea
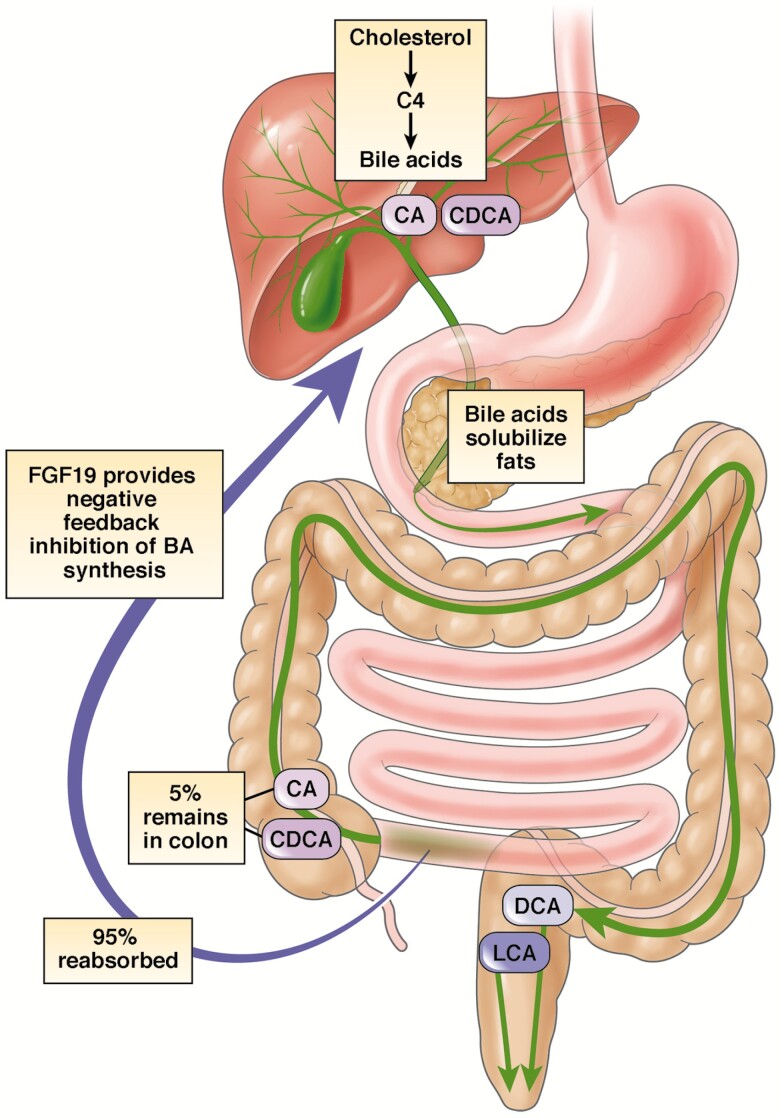
Bile acids are made in the liver to help digest fat.
Normally:
- bile acids leave the liver and gallbladder via the bile ducts and enter the intestine after meals
- they are reabsorbed in the last part of the small bowel called the terminal ileum
- they are recycled back to the liver
In normal function, bile acids also help regulate bowel function.
Recycled bile acids:
- help absorb dietary fats and fat-soluble vitamins (A, D, E and K)
- support nutrient absorption in the small bowel
- gently stimulate the colon
- help keep stool naturally hydrated and easy to pass
Small amounts reaching the colon are normal and beneficial. Everyone has bile acids contributing to healthy stool hydration and movement.
When the system becomes unbalanced
Bile acid diarrhoea is usually a problem of excess bile acid exposure, excess bile acid sensitivity, or both.
Bile acids normally stimulate water secretion and bowel movement. When excessive amounts reach the colon, or when the colon is unusually sensitive to bile acids, these normal effects become exaggerated.
This can:
- pull excess water into the bowel
- speed up gut movement
- increase urgency
- make stools loose or watery
- make bowel control more difficult
This is called bile acid diarrhoea (BAD), also known as bile salt diarrhoea or bile acid malabsorption.
Symptoms do not always perfectly match the degree of bile acid loss. Some people with relatively mild bile acid excess can still have severe urgency because their colon is particularly sensitive to bile acids.
How cholestyramine works
Cholestyramine is not absorbed into the body.
It stays inside the intestine and acts like a sponge, binding bile acids so they cannot irritate the colon.
Less bile acid reaching the colon leads to:
- less water secretion
- slower colonic stimulation
- firmer stools, helping to avoid distressing diarrhoea, urgency or accidental leakage
Importantly, cholestyramine works inside the intestinal lumen, including the small bowel, binding bile acids before they reach the colon where they cause diarrhoea.
Cholestyramine therefore becomes one valuable lever used to rebalance bowel function. It is mainly used when the problem is too many bile acids. However, because well-formed stools are easier to hold and control, in patients with accidental leakage or faecal incontinence it can also help improve control and reduce leakage.
How to use cholestyramine properly
How do I make sure I give it a good trial?
Cholestyramine can be very effective when used properly.
Most treatment failures occur because of:
Rapid dose escalation increases bloating and constipation, leading to poor tolerance and early discontinuation before therapeutic benefit develops.
Cholestyramine works best when it is present in the small bowel when bile acids arrive from the liver and gallbladder after meals.
-
Dose never increased enough
Bile acid load varies widely between patients, and many people require higher doses to bind sufficient bile acids for symptom control. An adequate trial means the right dose for at least 1–3 weeks.
Clinical improvement often takes time. If 16 g/day is your effective dose, it may take several weeks to reach and properly assess that dose.
This guide helps avoid those problems.
How to start cholestyramine
A gentle start improves tolerance.
Recommended starting dose
Begin with one sachet per day divided into two doses:
- half a sachet (about 2 g) before breakfast or lunch
- half a sachet (about 2 g) before the evening meal
Starting slowly reduces bloating and improves long-term success.
Increasing the dose
Increase every 4 to 7 days depending on symptoms and tolerance.
Typical progression (before or with food and before bed):
- Week 1: half sachet twice daily
- Week 2: one sachet twice daily
- Week 3: one sachet three times daily
- Week 4: one sachet four times daily
Continue gradual increases if needed to a maximum of 24 g/day (6 sachets/day), trialled for about 2 weeks at the maximum effective or tolerated dose before deciding it does not work.
How much do people usually need?
Across studies:
- 35 to 45 percent improve on 8 g/day or less
- 35 to 45 percent need 12 to 16 g/day
- 10 to 20 percent require 20 to 24 g/day
Dose requirement depends mainly on how much bile acid reaches the colon rather than body size.
When should I take it?
Bile acids are released after eating.
Take cholestyramine:
- 15 to 30 minutes before meals, or
- with the first mouthful of food if easier
Typical schedule:
- before breakfast
- before lunch if prescribed
- before dinner
- bedtime dose if prescribed
Consistency matters more than perfect timing.
Should I take cholestyramine at bedtime?
In selected cases yes.
Although bile acids are released after meals, many people continue to have bile acids entering the bowel between meals and overnight.
A bedtime dose may help if you have:
- morning urgency or diarrhoea
- symptoms not clearly related to meals
- previous ileal surgery or Crohn’s disease
- persistent symptoms despite daytime dosing
Typical example schedule:
- before breakfast
- before dinner
- bedtime dose if prescribed
The evening or bedtime dose often improves next-morning bowel control.
Your doctor will individualise timing depending on symptoms.
Taking cholestyramine with other medications
Cholestyramine can bind tablets and reduce absorption.
The simple rule
Take other medicines:
- at least 1 hour before cholestyramine, or
- 4 hours after cholestyramine
Be particularly careful with:
- thyroxine
- blood thinners such as warfarin, apixaban, rivaroxaban and dabigatran
- digoxin
- phenytoin or carbamazepine
- tacrolimus or cyclosporine
- oral contraceptive pills
Check with your pharmacist or doctor if unsure.
A practical schedule that works for most people
| Time |
Medication |
| Wake |
Morning tablets |
| Breakfast (1 hour later) |
Cholestyramine |
| Dinner |
Cholestyramine |
| Bedtime |
Evening tablets |
The goal is a workable routine, not perfection.
What if it does not work?
How long should I try it before deciding it works?
A fair trial means:
- regular daily dosing
- correct timing
- gradual dose adjustment
- enough time at an effective dose
Expected timeline:
- First few days: bowel adjusting, bloating possible
- Week 1 to 2: stools begin to firm, urgency improves
- Week 3 to 4: full effect usually clearer and the dose can be fine-tuned
A proper therapeutic trial usually means 3 to 4 weeks total, including at least 10 to 14 days at an adequate dose (often 8–16 g/day).
Stopping earlier risks missing benefit.
Why cholestyramine sometimes seems not to work
Most issues are fixable:
- dose started too high
- taken at random times
- stopped too early
- dose never increased enough
- fat intake remains high
- diarrhoea has more than one cause
- the powder is difficult to tolerate regularly
Partial improvement can still provide useful diagnostic information.
What if cholestyramine does not work or is hard to tolerate?
Not improving with cholestyramine does not always mean bile acid diarrhoea is the wrong diagnosis.
In Australia, Questran Lite® is available on the PBS and is usually much cheaper than compounded cholestyramine, colesevelam or newer off-label options. For most patients, it is therefore the practical first choice when a bile acid binder is needed.
Some patients use compounded cholestyramine if they cannot tolerate Questran Lite® or need a different formulation. This may be helpful for selected people, but it is usually more expensive as a private prescription.
If cholestyramine is not tolerated or does not provide enough control despite a proper trial, your doctor may consider other options. These may include:
- adjusting the dose or timing
- using a bedtime dose
- adding soluble fibre such as psyllium or PHGG
- trying a compounded cholestyramine preparation
- switching to another bile acid binder such as colesevelam, although this is usually more expensive
- adding an anti-diarrhoeal medicine such as loperamide in selected cases
- reassessing for other contributors such as microscopic colitis, coeliac disease, pancreatic insufficiency, Crohn’s disease activity or IBS with diarrhoea
GLP-1 medicines and other newer approaches are not standard first-line treatment for bile acid diarrhoea. They may occasionally be considered by specialists in selected refractory cases, particularly if there is another reason to use them, but cost, availability, side effects and indication need to be considered carefully.
The aim is not just to stop diarrhoea, but to find a practical and affordable routine that improves urgency, stool form and confidence with bowel control.
Diet strongly affects bile acid release.
Less than 40 g of fat per day (about 20% of calories).
Lower fat intake means less bile acid release.
Sometimes.
Soluble fibre can help improve stool form and bowel control. It works differently from cholestyramine. Cholestyramine binds bile acids, while soluble fibre can help absorb excess water, improve stool consistency and reduce looseness.
Psyllium is a gel-forming fibre that absorbs water and creates bulk. It is particularly helpful when the main goal is to bulk and firm loose stool.
PHGG is a water-soluble, non-gelling fibre that is usually easier to tolerate, particularly in people prone to bloating. It also has prebiotic properties that may support beneficial gut bacteria.
Important: avoid insoluble fibre such as wheat bran if you have diarrhoea, as it may worsen symptoms.
Fibre is usually an add-on, not a replacement for cholestyramine when bile acid diarrhoea is the main problem. It often works best when cholestyramine has already provided some improvement but stools remain somewhat loose or inconsistent.
Usually means the dose is slightly too high. Reduce slightly and increase more slowly if needed.
Common early and usually settles within one to two weeks.
Patients sometimes notice temporary bloating, fullness or mild constipation during the first week as the bowel adjusts.
Cholestyramine may reduce absorption of vitamins A, D, E and K.
Many patients who initially think it did not work achieve excellent control once timing and dosing are optimised.