Constipation and Bowel Leakage
A More Practical Way to Think About It
Many people are surprised to learn that constipation and bowel leakage often go together.
You might feel “blocked up” and still have accidents. Or you might be told your stool is “too loose” even though you don’t feel like you’re emptying properly. Both can be true at the same time.
The reason is usually not just the stool.
Very often, the real problem is that the rectum does not empty properly.
In short
Many people with constipation and bowel leakage don’t mainly have a problem with stool being “too hard” or “too loose”. The deeper problem is often incomplete emptying of the rectum. Old stool stays behind, the rectum becomes stretched and less sensitive, and softer stool can leak around what’s retained.
In these situations, simply adding fibre or laxatives can make leakage worse.
Treatment often works better when we focus on:
-
Emptying the rectum properly and predictably, and then
-
Keeping stool calm and controllable in between
Why constipation and leakage often happen together
Several common mechanisms tend to overlap:
-
Incomplete emptying → stool remains in the rectum
-
Rectal stretching and reduced sensation → weaker or delayed urge to go
-
Softer stool leaking around retained stool → “overflow” leakage
-
Weakened sphincter or pelvic floor muscles → less margin for error
This is why someone can be “constipated” and still have bowel accidents.
Many people experience this as a frustrating cycle:
“Blocked, then leaking — or loose and leaking — but never really in control.”
Why softening stool alone can make things worse
Fibre and laxatives are often helpful in simple constipation. But in people who also have bowel leakage, they can sometimes backfire.
This is because there are two different ways things can go wrong:
-
In some people, the rectum does not empty properly. Stool stays behind, and when it is softened it can leak around what is retained.
-
In others, emptying may be reasonably good, but the anal sphincter is not strong enough to reliably hold softer or looser stool.
In both situations, softening the stool does not fix the underlying problem. Instead, it can:
-
Make stool harder to hold in
-
Increase leakage or make it more unpredictable
-
Create a frustrating cycle of “easier to pass, but harder to control”
This doesn’t mean fibre or laxatives are “bad”. It means they need to be used for the right problem and in the right way, often as part of a broader plan that also addresses emptying and control.
A different way to think about treatment
For many people with constipation plus leakage, trying to make the bowel work “normally” every day doesn’t work well.
Instead, treatment is often more successful if we focus on two clear goals:
-
Planned, complete emptying of the rectum
-
Firmer, more controllable stool in between emptying days
Step 1: Planned, complete emptying
Rather than waiting for unpredictable urges, this approach means emptying the rectum on purpose, on a schedule.
The aims are to:
-
Properly clear the rectum
-
Reduce stool being left behind
-
Make bowel function more predictable
-
Reduce leakage between emptying days
Options can include:
-
Suppositories or micro-enemas used on planned days
-
Transanal irrigation (TAI), which gently wash out the rectum with water while sitting on the toilet
A helpful way to think about this is intermittent catheterisation for the bowel:
-
You empty it properly
-
At a time you choose
-
So it stays quieter and more predictable in between
This approach is not about forcing the bowel to behave “perfectly” every day.
It is about taking control of when and how emptying happens.
Important: Transanal irrigation is not a first-line treatment. It is usually considered when simpler strategies have failed and when symptoms suggest that incomplete rectal emptying is a major driver of the problem. It is typically taught, supervised, and tailored to the individual.
Step 2: Firmer, more controllable stool in between
Once the rectum is being emptied properly, the goal on non-evacuation days is:
-
Less urgency
-
Less leakage
-
Better control
-
More confidence going about daily life
This often means not keeping the stool as soft as possible.
Depending on the person, this may involve using:
-
Reduced daily doses of osmotic laxatives or stopping
-
Small doses of loperamide to firm stool
-
Cholestyramine if bile acids are contributing to loose stool
-
Moderate, not excessive, fibre
The aim is not to cause constipation, but to:
-
Keep stool formed enough to hold
-
Reduce seepage and accidents
-
Maintain comfort and predictability between planned emptying days
Putting it together
For the right patients, this approach often works far better than chasing a “perfect” daily bowel motion:
-
Empty properly and predictably
-
Then keep things calm and controllable in between
This is the logic behind structured bowel care plans and treatments such as transanal irrigation. They are not about being “more aggressive”. They are about being more deliberate, more predictable, and more humane.
When you should seek medical advice
You should seek medical review if you have:
-
New or worsening bowel leakage
-
Blood in the stool
-
Unexplained weight loss
-
Anaemia
-
Severe or persistent abdominal or rectal pain
-
A major change in bowel habit
-
Symptoms starting later in life
-
Neurological symptoms (such as leg weakness, numbness, or bladder changes)
A final word
Constipation with leakage is common, distressing, and often misunderstood. In many people, the key problem is not stool consistency, but how well the rectum empties.
With the right assessment and a plan focused on predictable emptying and better control in between, symptoms can often improve substantially.
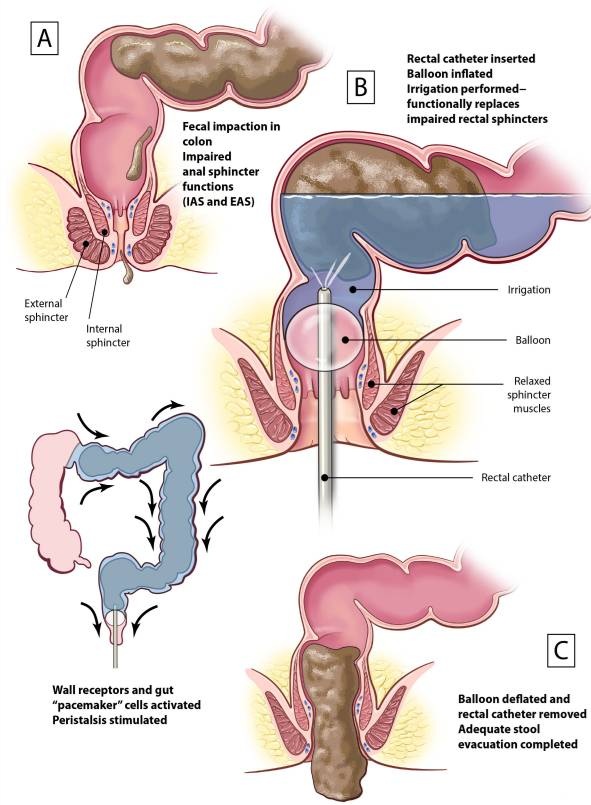
When Conservative Measures Aren’t Enough: The Next Steps
If changes to diet, fibre, laxatives, suppositories or enemas, and pelvic floor physiotherapy have not given you reliable control, bowel management usually follows a stepwise approach:
Diet and lifestyle measures
Oral and rectal medications
Transanal irrigation (TAI) when the main problem is emptying
Sacral nerve stimulation (SNS) in selected patients when the main problem is holding
Surgical options such as antegrade irrigation or a stoma
Each step targets a different problem: emptying, continence, or predictability.
In practice, this means there are three main evidence-based options to consider beyond conservative care:
Transanal irrigation (TAI)
A planned, mechanical way to empty the bowel and reduce unpredictable leakage.
Sacral nerve stimulation (SNS) - also called sacral neuromodulation (SNM)
A nerve stimulation treatment for selected people whose main problem is bowel control rather than emptying.
Stoma
A surgical option for severe, life-dominating bowel dysfunction when other treatments have not worked.
Which option is most appropriate depends on how your bowel is failing:
Is the main problem emptying?
Is it mainly holding?
Or is it both?
Option 1: Transanal Irrigation (TAI)
Transanal irrigation is usually the first of these options considered when the dominant problem is incomplete emptying with secondary leakage.
TAI is not experimental and not a last resort. It is recommended in multiple clinical guidelines as a second line treatment for complex bowel dysfunction, after conservative treatments and before surgery is considered.
It is widely used in neurological bowel disorders such as spinal cord injury, multiple sclerosis and Parkinson’s disease. The same bowel mechanics also apply to many people with:
Mixed constipation and faecal incontinence
Incomplete rectal emptying with stool build up
Overflow or passive leakage
Poor response to fibre, laxatives, suppositories, enemas and physiotherapy
What problem is TAI designed to solve?
In many people:
The rectum does not empty reliably
Stool accumulates
The anal sphincter does not seal well enough, especially for soft stool
The result is a familiar pattern:
“Blocked, then leaking” or “loose and leaking”, but never predictable.
TAI aims to:
Empty the rectum and lower bowel on purpose and on a schedule
Reduce stool retention and overflow
Reduce unplanned leakage between bowel actions
Restore predictability rather than relying on unreliable urges
What is transanal irrigation?
Transanal irrigation involves:
Placing a small catheter or cone into the rectum
Introducing warm tap water
Allowing the rectum and lower bowel to empty into the toilet
It is:
Taught by continence nurses or pelvic floor physiotherapists
Performed at home
Usually needed every one to three days once a routine is established
Common benefits include:
More complete emptying
Fewer accidents
Less reliance on laxatives
Better predictability and confidence
Many patients say:
“I didn’t realise how much of my leakage was from never really being empty.”
Is TAI safe?
TAI is generally safe when:
Patients are carefully selected
Structured training is provided
Early follow up is arranged
Common early effects include:
Abdominal cramping
Minor discomfort
Local irritation
Serious complications such as bowel perforation are very rare, estimated at around two per million procedures. They are most likely in the first few weeks, which is why supervised initiation and follow up are important.
Who benefits most from TAI?
TAI tends to work best for people with:
Mixed constipation and incontinence
Incomplete emptying with rectal loading
Overflow or passive leakage
Failure of conservative treatments
The motivation and capacity, with or without support, to use the system
Better outcomes are more likely when there is:
A mixed symptom pattern
Slow or prolonged colonic transit
Good engagement with training and follow up
When might TAI be less helpful?
TAI is less likely to help when:
The main problem is pure urgency with normal emptying
Diarrhoea is uncontrolled
There is no capacity to manage the equipment
Symptoms are mild and already controlled with simpler measures
Does TAI also help in non neurological bowel disorders?
Yes. While the strongest trial evidence comes from neurological bowel conditions, studies also show benefit in:
Non neurological chronic constipation
Mixed evacuation and incontinence patterns
Incomplete emptying after conservative treatments have failed
Even without a neurological condition, bowel dysfunction usually comes down to a small number of common problems:
Incomplete evacuation
Poor sensation or coordination
Pelvic floor dyssynergia
Weak sphincter function combined with soft stool
TAI helps by:
Clearing retained stool from the rectum and lower bowel
Stimulating evacuation reflexes
Reducing the reservoir for leakage
Creating predictable, scheduled emptying
This is why it can work in both neurological and non neurological bowel disorders.
The practical message
TAI is not a first line treatment and not a shortcut.
It is most appropriate when you have already tried, with proper support:
Diet and medication optimisation
Pelvic floor physiotherapy
Biofeedback where appropriate
Rectal agents and behavioural strategies
…and still have unreliable emptying, persistent leakage, or both.
In that situation, TAI offers a mechanical, predictable, evidence supported way to restore control when physiology alone has not been enough.
The goal
The goal is not perfect bowels.
The goal is:
Predictable emptying
Fewer accidents
Less time managing bowels
More confidence to live normally
For many people with mixed emptying and continence problems, TAI is the turning point that finally makes bowel care predictable again.
Option 2: Who is SNS for?
SNS is most appropriate when:
The bowel empties reasonably well
The main problem is incontinence (urgency, poor control, sphincter weakness)
Stool consistency can be kept reasonably formed
The goal is to improve control, not to mechanically clear the rectum
The patient shows a clear benefit during the crucial 1 to 3 week trial stimulation, typically defined as more than 50 percent improvement
In short, SNS is a control solution, not an emptying solution.
Why might SNS work?
It is thought to improve nerve signalling and coordination between the bowel, pelvic floor, and brain, helping restore better timing, sensation, and reflex control. It does not fix a blocked or poorly emptying rectum.
SNS helps a substantial proportion of people with faecal incontinence, though reported effectiveness varies depending on how success is defined and how long people are followed. The exact mechanism of action is still not fully understood. While SNS has regulatory approval and is widely used, high quality sham controlled trial evidence is limited.
Complication and revision rates are not trivial, with many series reporting adverse events or device changes in the mid teens to low 30 percent range. The two stage procedure (test and implant) can cause pain at the implant site, infection, skin irritation, and uncomfortable or unintended stimulation.
Why might SNS not work?
SNS is less likely to help if the main problem is emptying rather than holding. It does not remove retained stool, fix a narrowed outlet, or correct severe evacuation disorders. It may also be less effective when nerve damage is advanced, when symptoms are driven mainly by very loose stool or diarrhoea, or when there is severe combined emptying and continence dysfunction.
In some people, the nerve pathways simply do not respond in a durable way to stimulation, which is why not everyone improves and why a trial phase is used before committing to permanent implantation. For others, complications, discomfort, or loss of benefit over time mean that SNS is not a long term solution.
Option 3: When a stoma is considered
A stoma is usually considered when:
Symptoms are severe and life dominating
TAI and or SNS have failed or are not suitable
There is severe combined emptying and continence dysfunction
Quality of life remains poor despite best treatment
A stoma is not a failure. It is a deliberate choice for reliability and control when the bowel can no longer be made predictable enough.
The lived reality
Many people who choose a stoma later say:
“I wanted predictability more than normal, and I wish I had done this earlier.”
That captures the real trade off: function and freedom over anatomy.
The short version
TAI helps you empty
SNS helps you hold
Stoma gives you predictability and control when neither is enough
A note about new treatments
Faecal incontinence is rarely caused by just one problem. In most people, it reflects a combination of:
Nerve dysfunction in the lower spine and pelvis
Abnormal sensation and muscle control in the anorectum
Reduced ability of the rectum to store stool
Disrupted communication between the bowel, pelvic floor, and brain
Because of this, treatments that target only one part of the system often help some people, but not enough.
Procedures that bulk up or repair the sphincter can improve the barrier, but do not fix nerve or coordination problems.
Sphincter repair surgery often looks good at first, but long term results are disappointing, with many people losing benefit over time.
Sacral nerve stimulation (SNS) helps some people, but not all, and can have complications, and we still do not fully understand why it works when it does.
So while current treatments can be useful, none reliably correct the full, multi layered problem that causes faecal incontinence.
That is why there is growing interest in new, non invasive nerve stimulation treatments that aim to improve the underlying nerve signalling itself, rather than just treating one symptom or one muscle. Early studies are promising, but these approaches are not yet routine care.
For now, they represent hope for the future, not standard treatment, and a reminder that we still need better, more complete solutions.
